Today, as medicine progresses more and becomes more brilliant with each passing day, neurosurgery, as one of its most important branches, is in full bloom. This must be due to the fact that the brain is one of the most miraculous things that the world has ever seen.
Basically, there’s probably nothing so perfect like a human brain – anywhere. And this is why specialists who dedicate all their work and effort to this magnificent part of our body tend to come up with different ideas and innovative procedures. It’s not only innovative and unique – it also improves the quality of human life and awakens some amazing progress that we could only dream about decades ago.
Having this in mind, we’ve prepared three significant mini-stories about three phenomenal procedures that represent their most brilliant work. And well, it’s only a tiny part of all the things they can do.
Neurosurgical Epilepsy Treatment to Improve Life Conditions
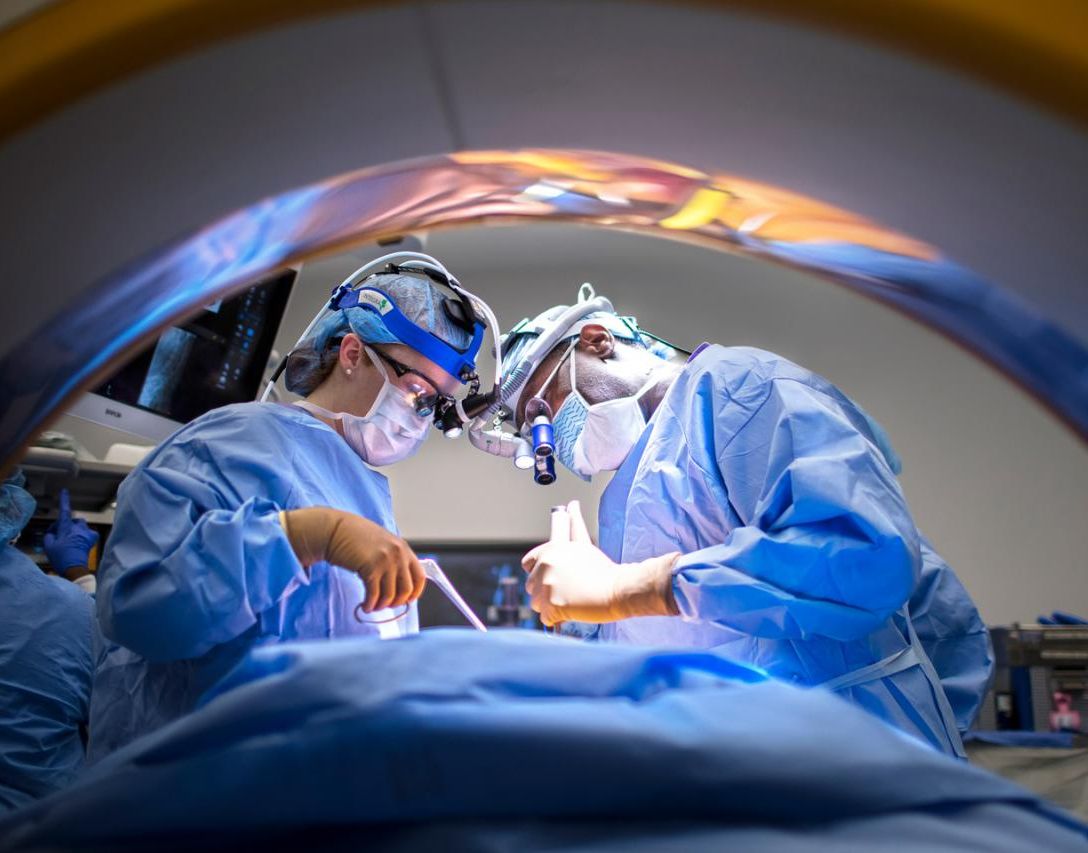
The main objective in the treatment of patients with epilepsy is to achieve adequate control of their seizures. These attacks sometimes affect patients more than expected. Of course, this process enables improving their quality of life and avoiding deterioration and exclusion associated with the presence of frequent and sustained epileptic seizures over years. According to brain-surgery.com, there are many people suffering from this kind of issue, it’s not difficult to conclude that this kind of brain surgery might save thousands of lives.
The optimal intervention would be the one capable of eliminating the generation of such attacks without producing unacceptable functional alterations, but sadly, this isn’t always possible. It can be said in broad strokes that there are two types of operations.
The first option, which could be considered curative, is aimed at suppressing the attacks completely, preventing the organism from having any further attacks. This is indicated in patients suffering from epilepsy in whom the epileptic focus is located in well-located brain areas. Therefore, it can be safely resected from it, not producing an intolerable neurological deficit.
On the other hand, there are palliative ones, in which due to the characteristics of the patient, only the number of attacks is considered to be reduced. The symptoms and their characteristics might be modified, but not completely cured. Palliative ones are performed in those patients who have several cortical areas with epileptogenic properties or who have the epileptogenic zone located in a region that simply can’t be resected
In order to be able to perform this process, there are two conditions that need to be fulfilled:
- The neurosurgeon should identify the location and extent of the epileptogenic area. The theoretical concept of epileptogenic zone is defined as the area of brain tissue necessary and sufficient to cause epileptic seizures.
- Assess the potential impact of surgery on the neurological function, cognitive performance, and emotional status of the patient. These are the factors that will decide which of two kinds of treatment will be performed.
Transplantation of Human Head to Cure Paralysis
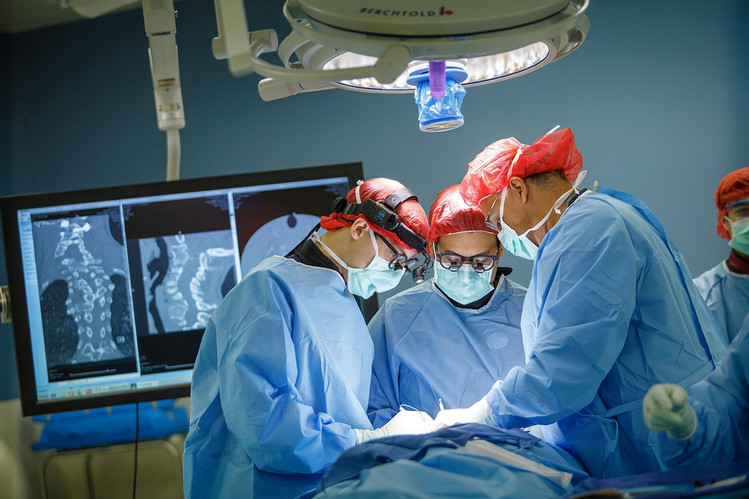
This idea DOES exist. And it’s not excluded that it might happen again and again, since this process seems to be an effective cure for a certain kind of paralysis which can appear as a consequence of neurological illnesses. The first operation suggestion like this happened in 2013 and it was given by a neurosurgical specialist from Italia, Dr. Canavero.
So, what was actually his idea?
He wanted to remove the head of the patient number one, who was healthy, but very carefully, taking care of performing the process as precisely as possible, as he wants to leave the spinal cord untouched and unhurt. Once he does it, he attaches the head to the body of the person that is paralyzed or suffers from any similar health issue.
This should be done by connecting the head and the body by after short-term hypothermia which needs to be performed in order to prevent nerves of any damage. Now, it has been proven that mammals can remain without blood flow for about sixty minutes, as long as the brain temperature is reduced to 12-15 ° C.
Under this hypothermia, neuronal activity can be recovered without noticeable damage once the blood circulation in the brain is restored. Therefore, Canavero proposed that two teams of perfectly synchronized surgeons should be available to work in the same room to section the respective donor and recipient head, lower the temperature of the brain to be transplanted and restore the blood supply in the latter once it’s sewn to the new body.
Of course, we don’t even need to guess how expensive and complex an operation like this would be. In addition to the list of candidates and the implicit difficulties of the surgery itself, there are other problems to solve in this type of interventions. Canavero estimates that the investigation to find an optimal method of transplantation could cost about 100 million dollars, would involve several dozen surgeons with other specialists and would continue for about 24 hours of procedures.
He was even announcing some attempts a couple of times, but a couple of volunteers simply gave up. And of course, they are not to blame; no one would feel completely relaxed about something like this, especially if it’s the first time ever. The only thing that remains is to wait and see if this marvelous doctor and his idea will come up with success in near future.
Deep Brain Stimulation for Reducing Symptoms of Parkinson’s Disease

Well, this one is not actually surgery, but it’s a job for neurologists and it’s absolutely amazing. The use of deep brain stimulation (DBS) as a therapeutic tool in Parkinson’s disease (PD) began in 1987 with the work of a team led by doctors Alim Louis Benabid and Pierre Pollak, in Grenoble, France. Its effectiveness quickly became evident, which is why it is now considered an essential therapeutic tool in the treatment of advanced PD1–4. Subthalamic nucleus DBS is a useful therapeutic tool for long-term motor complications, especially in the control of motor fluctuations and dyskinesias.
In idiopathic Parkinson’s disease, both the internal globus pallidus and subthalamic nucleus DBS have increased electrical activity as a result of damage to the nigrostriatal pathway, which can be inhibited by local electrical stimulation. Although high-frequency electrical stimulation reduces both motor symptoms and dyskinesias in both whites, it’s only in the subthalamic nucleus where stimulation can reduce the doses of levodopa and dopamine agonists necessary for good control of motor symptoms.
There are some general guidelines that guide us to the proper selection of patients who will have the greatest benefit of surgery. In this sense, we can distinguish some predictors of the benefit in surgery with young patients, those who have an excellent response to levodopa and those with motor complications – especially dyskinesia – as their main problem. These characteristics are met by approximately 10-15% of the population with Parkinson’s disease.
The follow-up demonstrates an excellent long-term response, especially in the control of motor aspects such as bradykinetic, stiffness and dyskinesias that is maintained over time. Sadly, the progression of the disease continues, but at least it’s possible to alleviate the symptoms and provide the patients with normal living conditions.